Baby Born After Five Blood Transfusions In The Womb
Hospital consultant says “It’s very unusual to see this so early on in pregnancy”
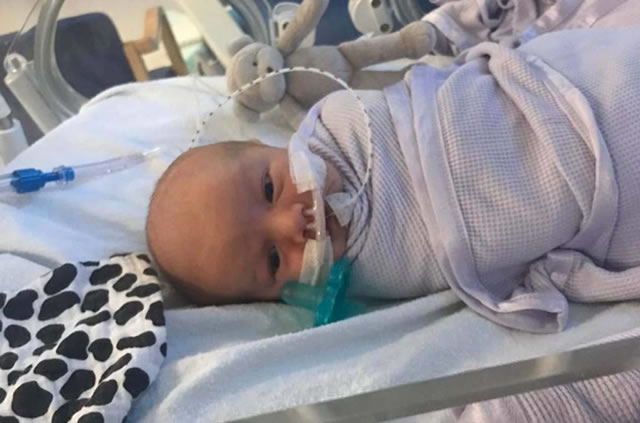
Baby Teddy
A baby with haemolytic disease of the newborn - a serious blood problem - who received five intrauterine blood transfusions from 20 weeks gestation, has been safely delivered at St George’s.
Baby Edward – known as Teddy – was born following complications during pregnancy, as mum Emma has rhesus disease meaning that while pregnant her rhesus negative blood attacked her baby’s rhesus positive blood cells.
Emma was referred to St George’s for specialist treatment and at 20 weeks gestation investigations raised a strong suspicion that Teddy was severely anaemic. He had developed ‘hydrops fetalis’, where skin swelling and fluid accumulation in his chest and abdomen meant there was a high risk he wouldn’t survive unless an intrauterine blood transfusion was carried out.
Transfusions come with risk at any stage of pregnancy, but particularly earlier on. At 20 weeks gestation the umbilical cord is only just large enough to manage receiving a transfusion.
Ahead of the procedure, Emma's blood was tested against the donor blood to ensure that there was a match and that her own blood would not attack it.
The transfusion was carried out via a needle being inserted through the Emma's uterus and into the 2-3mm vein of Teddy’s umbilical cord, guided via ultrasound imaging.
The transfused red cells typically last for 3-4 weeks, after which another procedure is required. Due to the nature of this procedure there are risks involved, including early labour or miscarriage, particularly when the baby is still developing at the earlier stages of pregnancy.
Emma and Teddy underwent three procedures before 24 weeks, the fourth was carried out at 28 weeks followed by the fifth and final intrauterine procedure at 32 weeks to ensure that he would be strong enough to be delivered at 35 weeks by caesarean.
Emma had previously researched rhesus disease and haemolytic disease of the newborn during her pregnancy with her two year old daughter Elizabeth* as she had also required two intrauterine transfusions for the same condition.
Emma, who lives in Cheam with her husband Gary and their two children, said: “I did a lot of research during my pregnancy with Elizabeth and found community groups of women with the same condition. I was very aware that lots of babies don’t make it, particularly those that have required transfusions so early on, like Teddy. We were completely in Dr Bhide’s hands and felt really reassured by the care he gave us and to Teddy.”
She said: “By Teddy’s last transfusion, we were just really looking forward to the delivery and meeting our little boy. We knew the transfusions had gone well so just hoped that he would be happy and healthy too.”
Dr Amarnath Bhide, Consultant in Obstetrics and Fetal Medicine at St George’s, said: “It’s very unusual to see this so early on in pregnancy. Usually we would do one, or possibly two transfusions in total starting from 28/29 weeks, so for baby Edward to have received five transfusions between 20 and 32 weeks is quite something.”
He added: “We chose to deliver Edward early as he was doing really well in the womb following the transfusions and undertaking another transfusion would have carried more risks than delivering him at 35 weeks gestation.”

Dr Amarnath Bhide, Consultant in Obstetrics and Fetal Medicine
who led Emma’s and Teddy’s care
Dr Bhide explained that on average, St George’s might see three to four women requiring similar specialist care every year, but that it is unusual for the transfusions to start so early on in pregnancy.
Following a short stay in the neonatal unit at St George’s, Teddy went home with his mum, dad and sister. Since his birth, he has needed an additional four blood transfusions which have stabilised his blood levels and he is a "happy, healthy little boy".
August 22, 2019
Related links
|